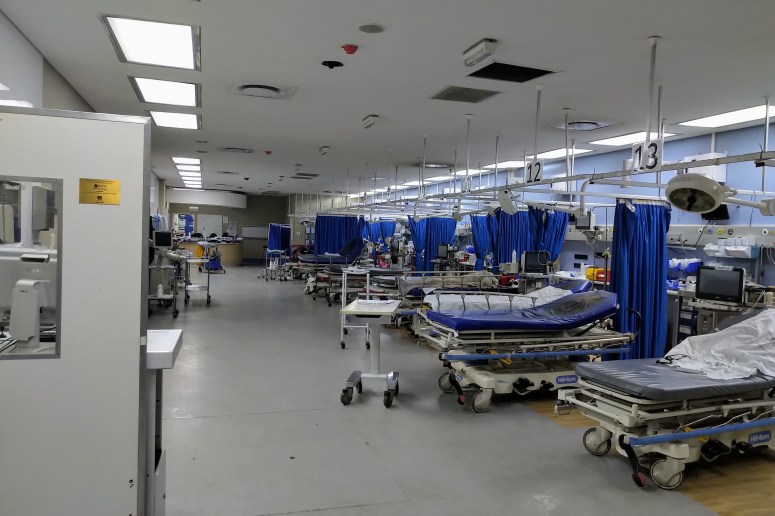
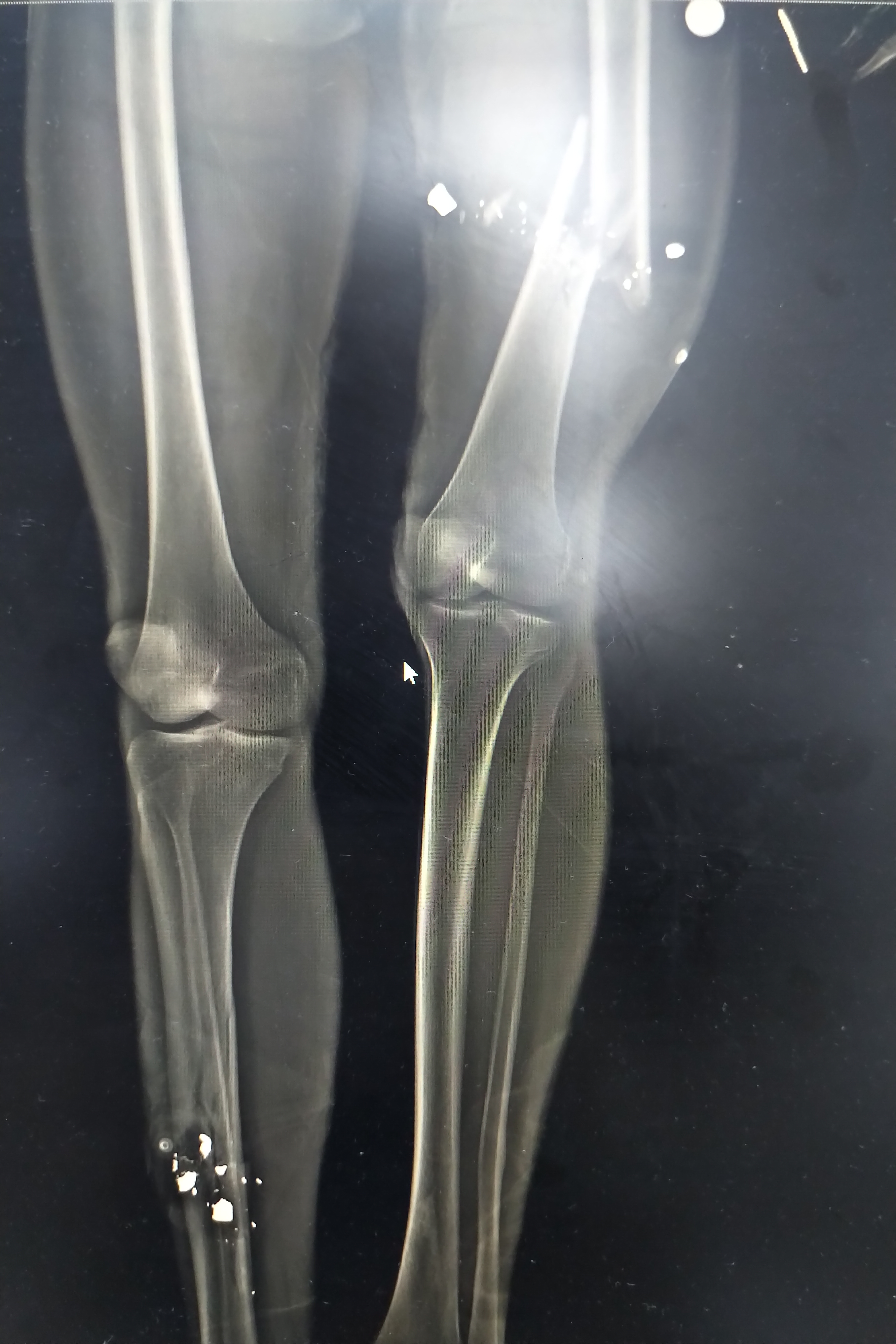
I did recently finish up my first elective rotation in Emergency and Trauma at Chris Hani Baragwanath “Bara” hospital. This is a gigantic hospital, largest in the southern hemisphere and third in the world, located on the edge of Soweto. Soweto “South West Township” is a massive township to the south west of Johannesburg’s core.
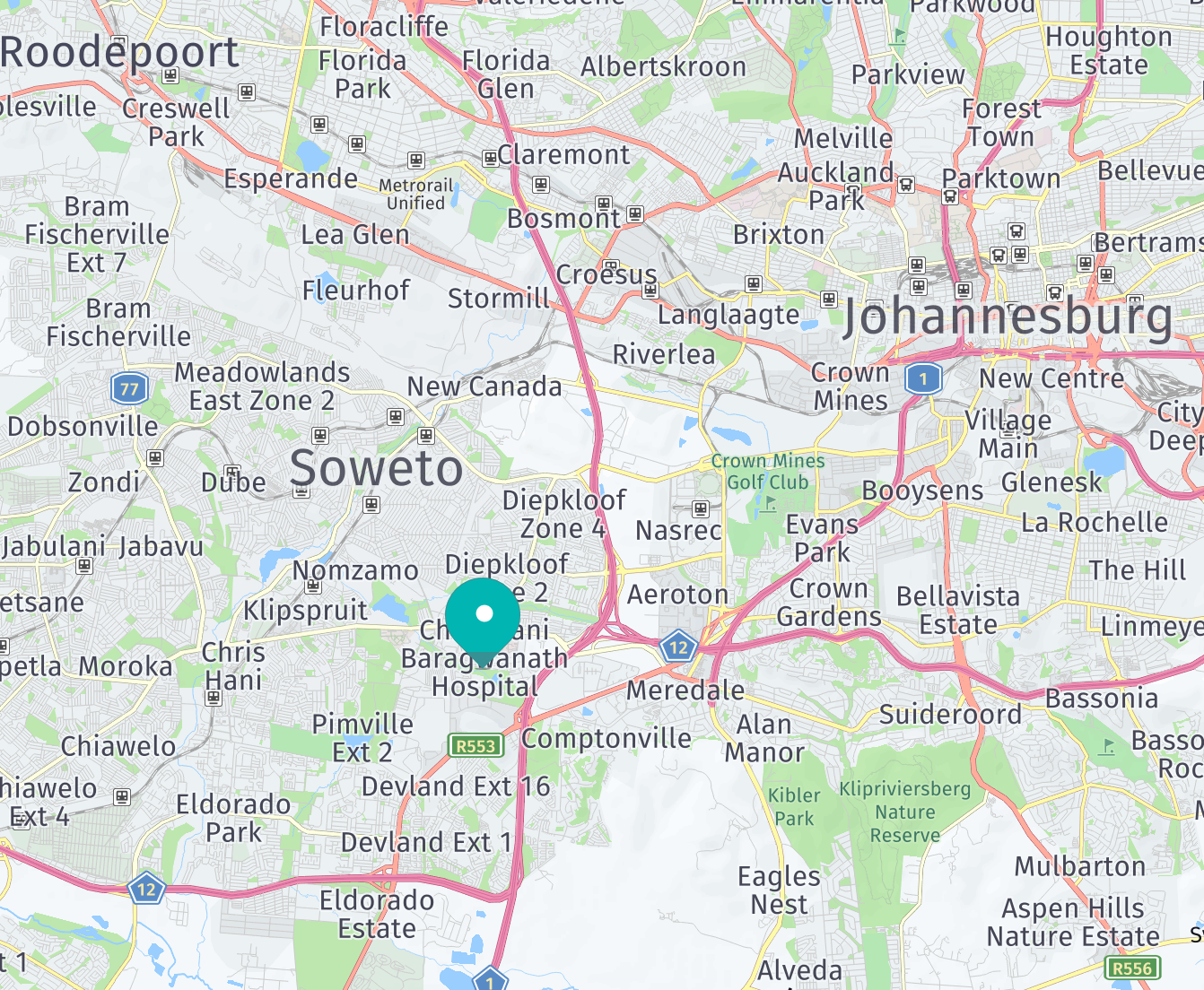

Though Soweto is technically part of Johannesburg, you won’t find many Sowetans who would agree with that. They are proud and independent. Unfortunately there is also significant poverty.
Medically, the location, specific social circumstances and resources of this hospital is part of what makes it such a good experience.
Location/System
Per above, Bara hospital is one of the few public hospital in Johannesburg. It is located on the Eastern outer edge of Soweto and so serves one of the most populous and impoverished areas of Jozi.
South Africa currently has a public/private healthcare system (possibly changing in the near future). There is significant disparity between the public system and the private; just as there is in the population at large. The public system is grossly underresourced, but persists admirably given the circumstances to serve a massive volume of people with significant medical needs.
Along with this disparity comes a stigma from patients to receiving care from the public system. I was told continually by people that they didn’t want to come to the public hospital, or didn’t want people to know they had come here. It was troubling and often led to patients arriving with delayed presentation of conditions that would have been much more readily reversibly if they were to present immediately.
Social Circumstances
This population suffers with significant weath inequality. Many of the have-nots are living in the townships and so are disproportionately represented in the population seen at Bara.
Medically this manifests as:
- Significant burns:
Much of the cooking is done using kerosene cooktops as most of Soweto lacks electricity. Very often we saw children with significant burns after the pot of food had tipped off the kerosene stove.
The homes are often built from tin fixed together into a box. They then insulate as best they can using plastic or cardboard on the inside. Again, their heating with kerosene open-flame often results in a fastly-spreading fire while they sleep and this burns can be severe. - Penetrating wounds:
Whether associated with robbery or general violence, the volume of penetrating wounds from knives, screwdrivers, machete or gunshot wounds is unbelievable. We would see 3-5 gunshot wounds per day as well as 10+ stabbings of one form or another. This is, of course, in addition to all the other general trauma.
The unique ubiquity of violence here has even shaped the hospital structure. Unlike anywhere I have been, Bara has two emergency departments in parallel. One is the medical emergency side which covers anything except trauma. This side has the usual three resusc beds. While the trauma side has two sections. ‘the pit’ is where patients go for suturing and fluid resusc. Three big sliding doors lead from the pit to the resusc area, which has twenty beds! - Suicide:
The number of attempted suicides we received were significant. Unfortunately the vast majority were in younger patients, particularly females. Most often the attempt was with (unique to me) toxins.
The most common were Organophosphates, Isoniazid, Tricyclics. - Traditional Healers:
While I have my concerns with many of the quackery in Canada, it is not often as damaging as these ‘sangoma’.
At least once a shift we would see a patient who had seen a traditional healer rather than visit the hospital or clinic for their illness. Most often they presented GCS 3 with fulminant liver failure. Unfortunately the usual tox screens were next to useless for the hepatotoxic substances these ‘healers’ were prescribing. And even if we could sort out the specific toxins, they were almost never reversible. These patients virtually always needed a transplant.
Resources
This was interesting to assess. Largely because they had some significant resources that you wouldn’t find in the smaller centres in Canada. Then on the flip side there were cheaper disposable items that we would regularly run out of during a shift, which would be unheard of back home.
Some examples of the big resources were:
This ‘Lodox’ machine. Located inside the doors of the trauma resusc area. This is a very fast full-body x-ray machine. You throw your poly-trauma or penetrating thorax patient up on here and you have many answers in 30 seconds.
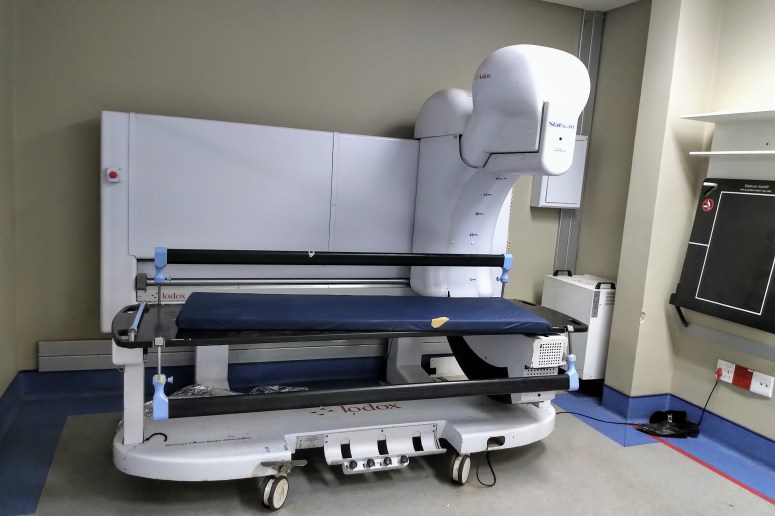
Three CT machines were available 24 hours a day, complete with angiography as well as an MRI.
The caveat is that they would often run out of seemingly insignificant parts that resulted in 2 of 3 machines being down for the majority of the time I was there.
In addition, we did not have a computer for viewing digital images. So we actually used the light boards on the wall or read the films against the ceiling lights. It made me nostalgic for a time that I never existed in.
They also had a blood gas machine in each emergency department. This was great because you could quickly grab some arterial gas and get nearly instant answer for electrolyte disturbances, lactate levels or any acidosis. I wish we had these available at home.
The more frustrating resource issues came from a lack of supply of basics. These were often: gloves, alcohol wipes, tegaderm for IV/CVC sites.
Staffing of course was another difficulty. Part of this, I believe, comes from the fact that the private sector pays far better. This affected both physicians and nursing. A side effect of the shortage of attendings and registrars meant that a real reliance on the students was present. This was nice from a learning perspective as you could see that your efforts actually mattered in keeping the queue outside as short as possible.
Nursing was often so stretched, eg 1:4 even in resuscitation. As a result we were often left fulfilling some of these functions on our own. For example, more often than not, I would end up doing my own blood draws, my own arterial bloods, setting up IV fluids, putting in foleys and running blood gases or pushing drugs. I enjoyed this for the short time as I was happy to learn these tasks, however, I can imagine becoming frustrated with it over time and it slows your ability to get to more patients.
Summary
Bara and South Africa in general was a wonderful experience. The registrars and consultants were all hungry to teach, the patient cases were unlike anything I will see in Canada and the procedures were manifold. I felt as though we were able to actually provide benefit through our work while at the same time gaining incredible experience.
I can’t imagine any other elective would have allowed me to get multiple central lines, intubations, chest tubes and lumbar punctures in such a short period of time and I do feel like it gave me a leg up from this perspective. I also gained a renewed appreciation for our public health system as well as the wonderful allied health colleagues: RT, nursing, OT, Social work.
Videos:
- This is the walkway up from parking in the back. It passes by the wards. Each ward is numbered and represents one of the single storey red-brick buildings. The hospital is actually a converted barracks with the modern ER built onto the front.
When you go into the wards you get a glimpse into the military origins. Each ward is wide open with cots along either side, just as you would see in military hospitals back in the day. - The approach to the hospital upon entering Soweto from Mondeor to the East.